The ministry of doctors without families
In Portugal, more than 1.5 million patients registered on the National Health Service have no GP. But, in the last decade, the number of specialists trained in general and family medicine has increased. If this is so, why is there a shortage of doctors in primary care?

© André Carrilho/Divergente
Since she was small, Patrícia Caeiros had dreamed of being a biologist, “like those you see on National Geographic”. She went on to study Veterinary Medicine and spent five and a half years in amongst the animals, but in the end, the low wages and difficult career progression caused her to change course. She told us that, at the time, she had two options: “emigrate and not come back, or make a life change”. She chose the second, and today, at 38, she is in her final year of general and family medicine specialty training. In just a few months she will be a qualified GP.
In the last decade, the number of specialists trained in general and family medicine has risen in Portugal: at the end of 2024, there were 9,343 active licensed doctors in this specialty in Portugal, 46% more than the 6,392 registered in 2015. These numbers stand in contrast with the perceived shortfalls and leaves the question: if there are increasing numbers of clinicians trained in family medicine, why is there such a shortage in health centres?
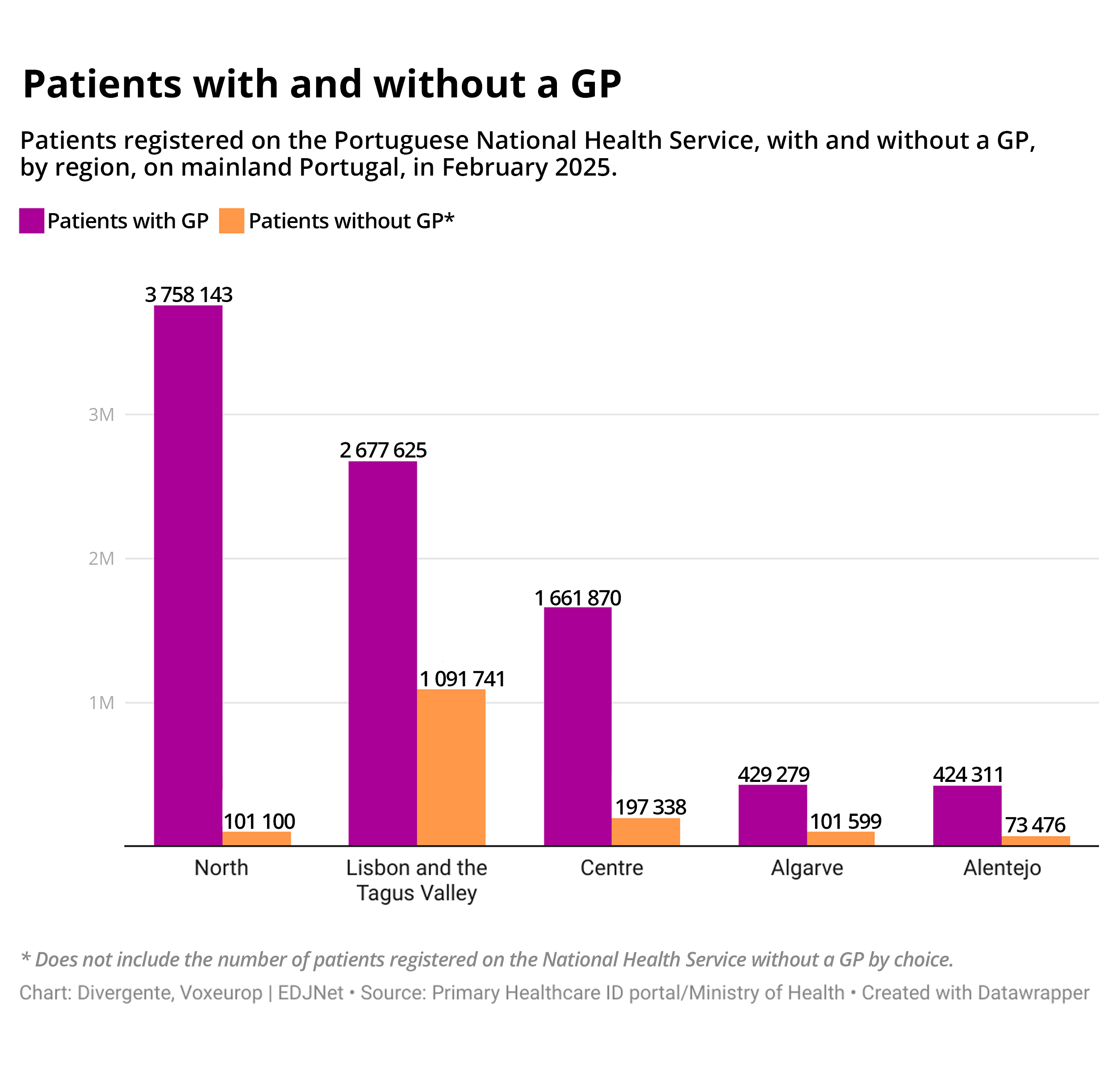
Let’s take this in stages. If we look at the numbers, over 15% of the people registered on the Portuguese national health services (mainland and the islands) have no GP. At the end of February 2025, that equates to 1,565,254 patients in this situation on mainland Portugal; on the same date, there were 5,411 clinicians registered to this specialty hired by the National Health Service across various primary healthcare centres.
The problem isn’t limited to us—looking across Europe, as Voxeurop and the European Data Journalism Network (EDJNet) did, we see that the GP shortage is a continent-wide problem, despite increases in trained professionals in the majority of countries analysed.
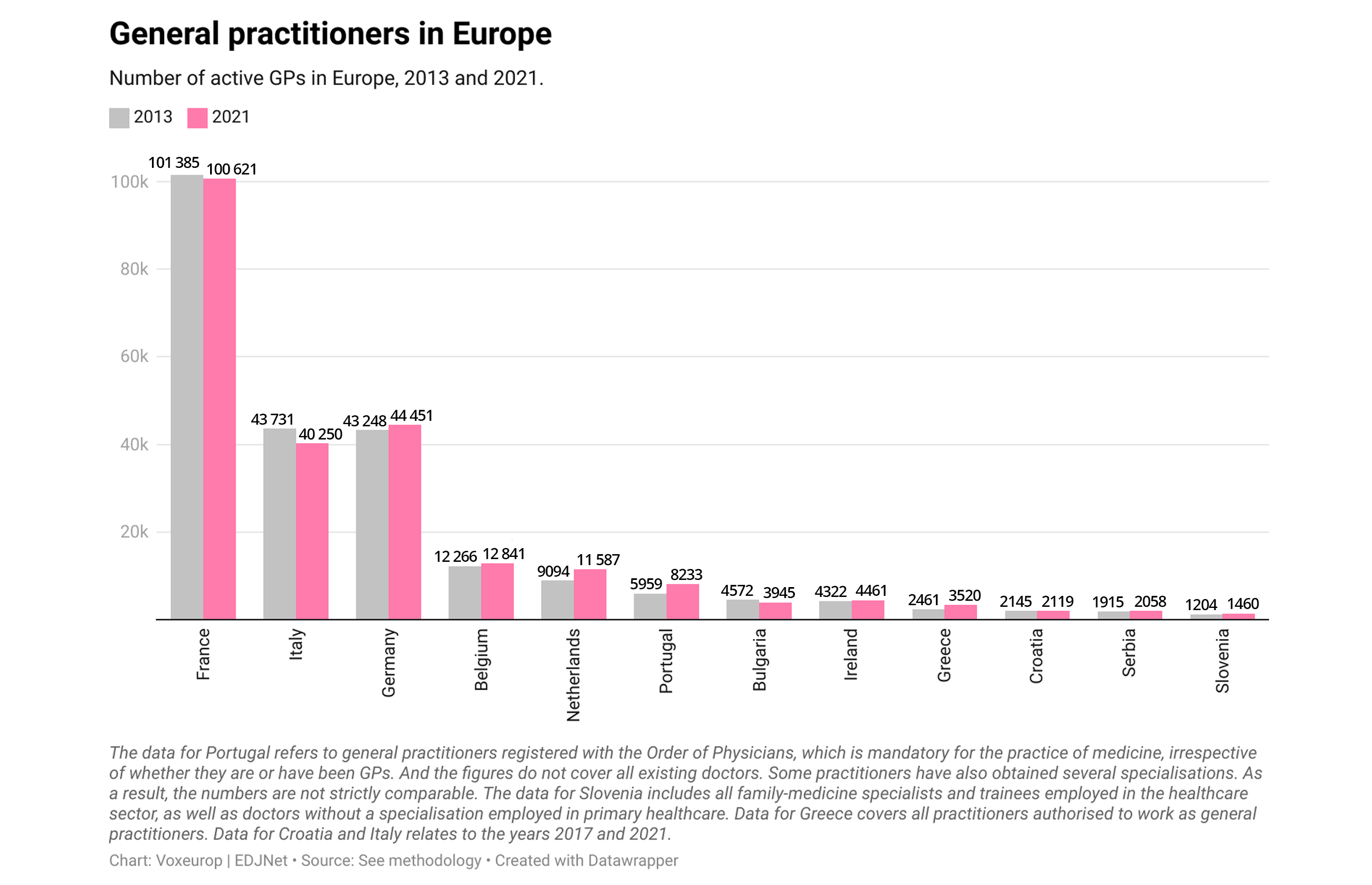
This shortage has consequences: when someone has a health problem, the first point of contact is primary care. Without them, there are many illnesses that may go untreated for years. The World Health Organization defends primary care as “the most inclusive, equitable and cost-effective way to achieve universal health coverage”.
Patrícia Caeiros is doing her training right in the eye of the storm, in the Tapada Family Health Unit in the parish of Algueirão-Mem Martins (Sintra), just northwest of Lisbon. In theory, everyone registered at a Family Health Unit is entitled to a GP, but in reality, it is not that easy. All you need is for a doctor to get sick, become pregnant or need to care for a relative for coverage to become an issue. Where Patrícia works there are five doctors and five nurses to treat 9,818 patients; only two patients have no doctor, and one by choice. A nugget of calm, like in the eye of a cyclone.
Outside, chaos awaits. Lisbon and the Tagus Valley has the worst GP shortage. And the people living in the municipalities of Alenquer, Arruda dos Vinhos, Azambuja, Benavente and Vila Franca de Xira who receive the worst treatment, where there are more people without a doctor (120,866) than with one (118,656). According to Ministry of Health data, in February there were just 71 general and family medicine specialists across these municipalities to serve 239,865 registered patients—a ratio of more than 3,300 people per doctor.
She is just months from her final specialty training assessment, the last step in becoming officially recognized as a GP, but Patrícia’s future path will not help to reduce the list of people without a doctor. “I will most likely provide locum services to the National Health Service, to have hours that work for me”, she says. Because going to work for a Family Health Unit, with a full-time contract, would mean having at least 1,750 patients and, in practice, never less than 40 hours’ work per week.
She will become another “bank doctor”, adding to the list of professionals who have filled the holes of the chronic staff shortages at the National Health Service. According to the Central Administration of the Health System, in 2024 the state hired agency doctors for a total of 5.1 million hours (a large proportion of which were for accident and emergency) and paid 213 million euros for this, the highest cost in the last three years.
Patrícia Caeiros did not set out to become a bank worker. As an activist for the right to health—she has already been on missions in the Mediterranean and Timor-Leste—she would prefer a part-time contract, with the proportional reduction in patients. “Why do they refuse to do this? By refusing, they pay a lot more to hire in bank doctors. It makes no sense!”
Part of the answer can be found in the law regulating Family Health Units. They can only hire doctors on a part-time contract in exceptional circumstances, “when a full-time contract is not justified”, and for no more than a third of doctors on the payroll.
This March, more than 400 medical students took exams throughout the country. If it goes well, in about a month, their results will be confirmed and a new intake of doctors recently specialized in general and family medicine will be ready to work. The law states that, 30 days after result confirmation, the Ministry of Health opens the calls. But the most recent ones have gone badly: in 2024, 70% of places were left unfilled; and in 2023, less than a third were taken.
Could it be the heavy workload, the lack of flexibility and the expectation of meeting unrealistic performance targets that makes it so difficult to shrink the list of people without a GP?
The president at the General and Family Medicine Specialist Branch of the Portuguese Medical Association has no doubt that these are decisive factors. Paula Broeiro believes that the current model for Family Health Units in Portugal, as it is designed, does not work. “I am 61. Now, I only work 35 hours per week, with 1,500 patients. I have labour rights, but the younger doctors have to work a lot to take home a decent wage. If they don’t want to face salary reductions, they are forced to meet indicators that, in the end, depend on the performance of the whole team. Managers do not understand that it is better to have two doctors hired part-time than having none. The younger generations want to be their own bosses. If I was 20 or 30, I might not be here either”, she says, half joking.
Patrícia Caeiros did not hear what the veteran said, but her words come from the same place. “I am much better off as a doctor than a vet, but life is for more than just working.”
*At the beginning of March, DIVERGENTE sent the Central Administration of the Health System a series of questions: How many GPs were employed by the National Health Service in the last 10 years? How many retired? How many bank doctors are working in primary care? And what is spent on these professionals? Despite insisting, as we send out this newsletter we are still waiting for answers.
